Male Genitourinary Disorders: Prostatitis
Prostatitis

Click on the name below for expert medical information & advice

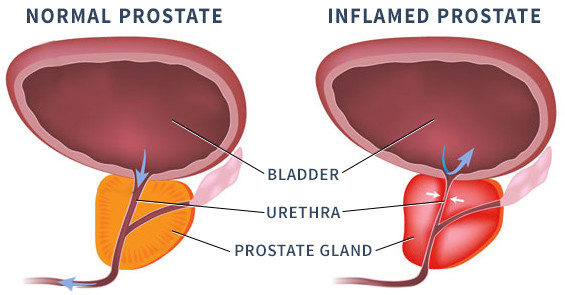
Prostatitis is the name given to a set of symptoms which are thought to be caused by an infection or by inflammation of the prostate gland.
Prostatitis is not a form of prostate cancer. It is also not the same as having an enlarged prostate.
It’s a common condition which can affect men of any age, but it’s most common in younger and middle aged men, typically between 30 and 50.
Prostatitis can cause a wide range of symptoms, which vary from man to man. Common symptoms include problems passing urine and pain or discomfort around your testicles, back passage or lower abdomen.
It’s a complicated condition. There are four types of prostatitis, listed below. Some types are not well understood, which make it difficult for doctors to know what causes it and know how best to treat it. This can be frustrating for men who have it, but there are things you can do to help yourself.
For more practical tips read our How to manage chronic prostatitis guide.
Signs and symptoms
Prostatitis can cause a wide range of symptoms, which vary from man to man. Some common symptoms include:
- discomfort, pain or aching in your testicles, or the area between your testicles and back passage (perineum), or the tip of your penis
- discomfort, pain or aching in the lower part of your stomach area (lower abdomen), your groin or your back
- needing to urinate frequently or urgently
- pain or stinging during or after urinating
- feeling as if you’re sitting on a golf ball
- no desire for sex (lack of libido)
- less commonly, difficulty getting or keeping an erection (erectile dysfunction), pain or burning during ejaculation, and premature ejaculation.
The different types of prostatitis can also cause other symptoms. Acute bacterial prostatitis can cause pain in your muscles or joints in the pelvic area, thighs and lower back. It can be severe, causing a high temperature (fever), sweating and chills. Some men find they suddenly and painfully can’t pee (acute urinary retention) – this needs treating straight away, usually at a hospital.
Chronic pelvic pain syndrome (CPPS) usually causes pain in the pelvic area (the area below your stomach), including the area between your testicles and back passage (perineum). The symptoms can go on for a long time. You might be diagnosed with CPPS if you’ve had symptoms for more than three of the last six months.
Speak to you GP if you have any of the symptoms listed here.
We are here to support you
If you are concerned about prostate cancer or prostate problems we can help. We provide a range of information and support so you can choose the services that work for you. All our services are open to men, their family and their friends.
Please visit : https://prostatecanceruk.org/get-support
Or you can speak to specialist nurses on:
0800 074 8383
*If you are unsure about the cause of any pain ensure you speak to a doctor or nurse at your haemophilia centre immediately.

Seminal vesiculitis
Inflammation of the seminal vesicles is known as seminal vesiculitis. Seminal vesiculitis commonly occurs secondary to prostatitis; however, it can occur independently too. Prompt treatment of prostatitis should be done in order to prevent the progression of prostatitis into seminal vesiculitis.
Classification and Types of Seminal Vesiculitis
There are two types of seminal vesiculitis: Acute and chronic seminal vesiculitis. Seminal vesiculitis often occurs with prostatitis. The main symptom is hematospermia, i.e., sperm is either mixed with red or coffee colored blood.
Causes of Seminal Vesiculitis
The causes of vesiculitis are many including bacterial, viral and other unidentifiable causes. Some of the causes and risk factors of seminal vesiculitis include:
- Bacteria which may enter the seminal vesicles via urethra.
- Inflammation of the testis or epididymis can spread locally and lead to seminal vesiculitis.
- Infection of the prostate, rectum or bladder can spread directly to the seminal vesicles and cause seminal vesiculitis.
- Other infections or lesions, such as tonsillitis and gingivitis may also cause seminal vesiculitis, as the bacteria travels through the blood vessels.
- Factors which cause congestion of prostate or seminal vesicles can result in acute seminal vesiculitis, such as excessive alcohol intake, suffering from cold, excessive sexual intercourse, damage to the perineum area and prolonged pressure.
- Any obstruction of blood to the perineum area.
- Excessive heat in the body.
You can read further information here:
https://www.epainassist.com/pelvic-pain/testicles/seminal-vesiculitis




Source: Prostate Cancer UK / ePain Assist
